THE SAME CARE, DIFFERENT NAME
Kindred Pelvic & Children's Health was previously known as Cara Richmond Physiotherapy.
Where health feels human. Every kind. Every step. Every body.
Care beyond the clinic.
Expert Pelvic & Children's Health Physiotherapy in Melbourne.
Supporting pelvic health, pregnancy, postnatal recovery, children's continence/toileting, pelvic pain with personalised, holistic, evidenced based care.
Pelvic Health Expert Physiotherapists - Pregnancy & Postnatal Care - Children's Continence & Toileting Support - Pelvic Pain - Prolapse - Exercise & Rehabilitation

Founded by Cara Richmond, Kindred Pelvic & Children’s Health was previously known as Cara Richmond Physiotherapy.
In early 2026, we changed our name to better reflect our growth and commitment to providing inclusive, specialised physiotherapy services for individuals of all genders and children across various Melbourne locations, including Bundoora, St Albans, Werribee, Spotswood, and Ascot Vale.
Our Services
WOMEN
- Incontinence and bladder leakage management
- Pelvic organ prolapse support
- Pelvic floor dysfunction assessment and treatment
- Pelvic pain, including endometriosis and vaginismus
- Bladder and bowel health concerns
- Individualised, evidence-based care to reduce symptoms, restore function, and help you feel confident in your body again.
CHILDREN'S TOILETING
- Constipation management and bowel health support
- Bedwetting (nocturnal enuresis) treatment
- Toileting challenges, including toilet training support
- Bladder and bowel continence care for children
- Support for neurodivergent children with tailored, individualised approaches
- Positive, practical strategies to build confidence and independence
- Compassionate, supportive care to help children and families develop healthy, sustainable toileting habits.
PREGNANCY
- Pregnancy care and birth preparation
- Postnatal recovery and abdominal separation
- Pelvic floor support
- Joint aches and pain management
- Safe return to exercise
- Support to help you feel strong, prepared, and confident through every stage.
POST NATAL
- Postnatal recovery and rehabilitation
- Abdominal separation (diastasis recti) assessment and core strengthening
- Pelvic floor assessment and retraining
- Management of post-birth aches, pains, and musculoskeletal changes
- Guidance for a safe return to exercise and everyday activities
- Support and recovery from mastitis and nipple trauma
- Strategies for safe feeding positions, pain relief, and ongoing breastfeeding
- Personalised, compassionate care to help you regain strength, confidence, and wellbeing after childbirth.
ADOLESCENT PELVIC & PERIOD PAIN
- Support for adolescent pelvic pain and menstrual-related discomfort
- Guidance for managing painful periods (dysmenorrhea) and irregular cycles
- Pelvic floor assessment and gentle retraining
- Education on posture, core strength, and self-care strategies
- Strategies to improve comfort, confidence, and daily function
- Evidence-based, compassionate care to help adolescents manage pelvic pain, understand their bodies, and feel empowered.
MEN
- Assessment and management of pelvic floor dysfunction
- Support for bladder and bowel concerns, including incontinence
- Recovery and rehabilitation after prostate surgery
- Management of chronic pelvic pain and sexual pain
- Guidance on core strengthening, posture, and pelvic floor exercises
- Evidence-based, individualised care to help men improve pelvic function, reduce symptoms, and regain confidence in daily life.
TRANSGENDER PELVIC HEALTH
- Support for pelvic floor function and core strength
- Management of bladder, bowel, and continence concerns
- Guidance for post-surgical rehabilitation (e.g., gender-affirming surgery)
- Assistance with pelvic pain, sexual health, and core stability
- Individualised, affirming care tailored to gender-diverse needs
- Compassionate, evidence-based physiotherapy to help transgender and non-binary clients improve pelvic health, function, and overall wellbeing.
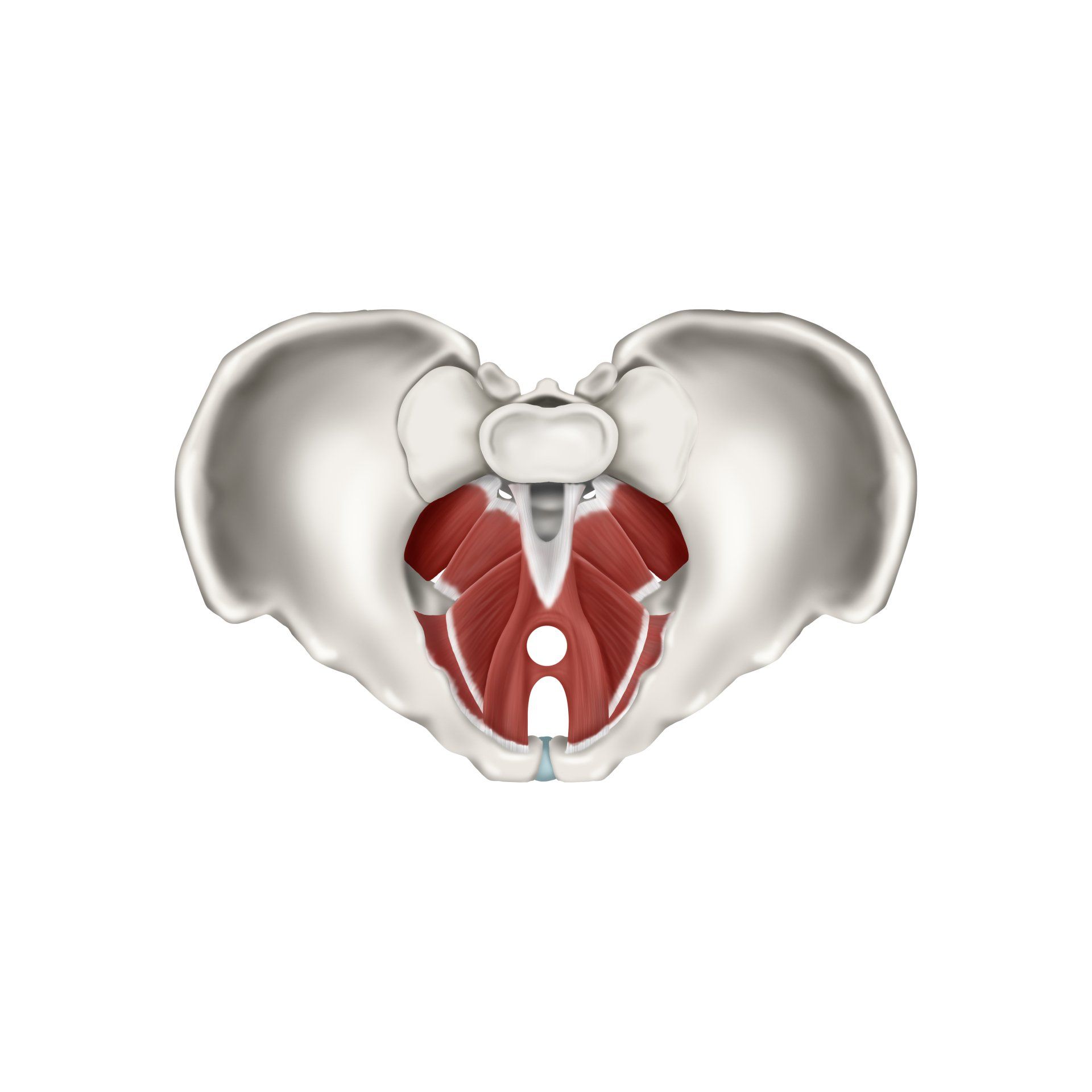
PELVIC FLOOR
- Assessment and treatment of pelvic floor dysfunction
- Support for urinary incontinence, bowel leakage, and constipation
- Management of pelvic organ prolapse
- Relief from pelvic pain, pelvic tension, and discomfort during sex
- Guidance for postnatal pelvic floor recovery and strengthening
- Core stability, posture, and functional movement retraining
- Education and exercises to prevent future pelvic floor issues
- Our evidence-based, individualised care helps men, women, and transgender clients improve pelvic function, reduce symptoms, and regain confidence in everyday life.
NDIS ASSESSMENT & REPORTS
- NDIS continence assessments for bladder and bowel support
- Individualised care plans aligned with NDIS goals
- Detailed reports for NDIS planners, support coordinators, and allied health
- Ongoing progress reviews and plan adjustments
- Practical strategies to build independence, confidence, and wellbeing
- Clear, compassionate, and evidence-based continence support for NDIS participants.
WHO WE HELP
• People experiencing pelvic pain or discomfort
• Pregnancy and postnatal recovery
• Children with toileting or continence concerns
• Individuals with bladder or bowel dysfunction
• People wanting to improve pelvic floor function
What to Expect
1. A private, respectful and thorough assessment.
2. Clear understanding of your symptoms and contributing factors.
3. A personalised treatment plan tailored to your goals.
Pregnancy and Pelvic Health Diaries


Follow us:
Instagram/Facebook @kindredpelvic
Tik Tok: @physiomamacara
Want some of our latest updates, recovery tips and pelvic floor advice?
Join our mailing list!
We will get back to you as soon as possible
Please try again later